By Rachel Broudy
Sixteen years ago, Dan Buettner studied the places in the world where people lived the longest. He went to the communities where people outlived their neighbors, with greater numbers of people living into their 90s and 100s. He called these the Blue Zones. As Mr. Buettner explored the Blue Zones, he found behaviors and qualities that ran through these communities and distinguished them from other communities nearby. His research and the stories of these communities suggest that the pathway to better health, longer life and, perhaps most importantly, better quality of life during our later years, is not more medications or improved health care delivery. Instead it is something else – something that we think of as wellbeing. It is about belonging in our communities, being connected to family and friends, and having meaning, purpose and engagement in our lives.
He went to Okinawa, Japan, where older adults talk about “ikigai,” or “that which makes one’s life worth living.” He found that people maintained routines that included daily visits with family and friends. Having tea is a way to stay connected with friends and engaged in community. In Sardinia, older adults live within extended families, where they still have a role and may walk the hills, tending the sheep, alongside younger herders and farmers. In the United States, Seventh Day Adventists live longer than their neighbors. They attribute their health and longevity to their faith, a greater purpose, as well as a practice of healthy eating and an active lifestyle.
In every single one of these communities, older adults had a role, a community to which they belonged, a place where they were seen and valued. Their lives in their later years were contiguous with their younger years. They lived well and fully, and it appears that meaning and connection may well have been driving their health, longevity, and wellbeing.
Why does this matter? It suggests that our current health care interventions for older adults may be geared towards the wrong variables. It suggests that quality of life – purpose, connection, meaning, and role – may do more for our health and longevity than many standard medical interventions. In fact, our traditional medical interventions may actually undermine the very things that we know create health and wellbeing. If you look at nursing homes, people live separated from their community, often without a role or purpose that is contiguous with their past selves; the focus of their care is primarily medical management and safety. Perhaps we need to rethink what creates health and how best to support it in older adults. There is no group for whom this issue is more relevant than older adults living in nursing homes.
There was another provocative study done by Ellen Langer at Harvard University. She performed a study in a nursing home on two dementia units. She was studying autonomy. For her intervention, she gave nursing home residents a plant to care for. They had to put it where they wanted in their room, water it and attend to it. They also had to choose which activities they wanted to attend and talk with a staff member to arrange a reminder plan for those activities. The control group also received a plant, which the staff cared for and placed on the windowsill. And the staff encouraged the control group participants to attend all the activities. There was a mortality difference! People who had control over their day and a plant actually lived longer than the control group. They also were happier and more active in the activities offered at the facility.
Again, this raises the question, to improve health and wellbeing for older adults, especially for those living in long term care, are we pressing on the right levers? And are we measuring the right outcomes? Do we think their care plans should be organized by medical diagnoses and interventions? Should our care instead be explicitly geared towards a goal of improving quality of life and wellbeing?
A team at Ariadne Labs is currently exploring this very question. This team of researchers has developed a model of wellbeing that emphasizes social connection, meaning, autonomy, and security.
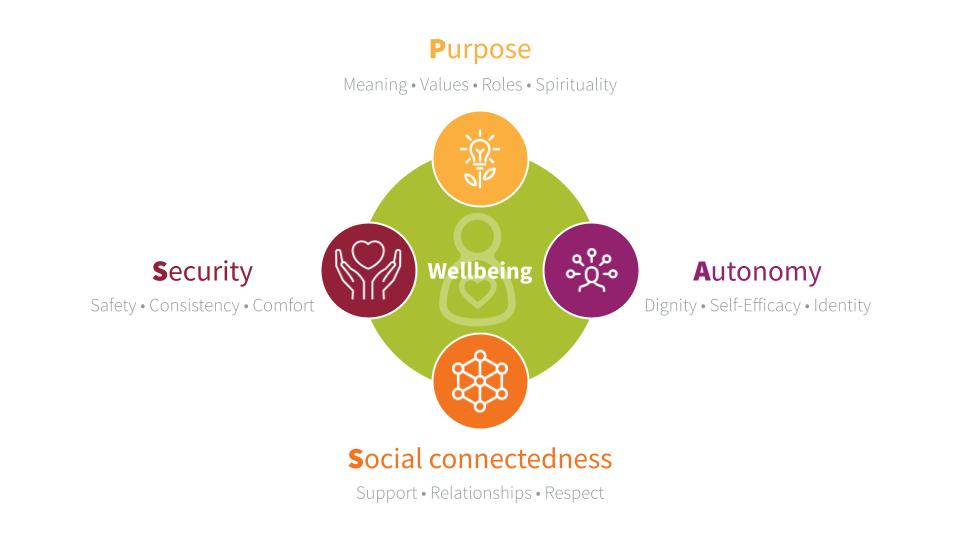
This model of wellbeing draws from evidence, experiments and anecdotes around quality of life and clinical outcomes in the care of older adults. The model focuses on these four areas as critical determinants of quality of life and also as opportunities for care interventions and support that improve quality of life. The Ariadne team is exploring how to learn what contributes to the wellbeing of individuals living in long term care and how to create and develop interventions that support wellbeing. Then, we will test these learnings to see if this kind of an approach improves clinical outcomes.
There is a great deal of evidence already that attending to quality of life improves clinical outcomes in long term care. This has been shown in Green House models and the Eden Alternative. When long term care residents feel connected to those around them, when their environment feels like home, when they feel engaged and cared for, they do better. And, not surprisingly, the staff are happier too. The retention rates at facilities where quality of life is a main focus and mission, are higher than at traditional nursing homes.
It has been challenging to scale Green House and Eden facilities, largely because the process is long, complex, and capital-intensive. As we enter yet one more surge of COVID-19 and the global pandemic, I am thinking about all the nursing home residents who were referred to my hospice organization with a diagnosis of failure to thrive. These were people dying of isolation and lack of connection. We all did our best in a novel and terrifying crisis to keep older adults alive in the face of COVID-19, but now we have yet more evidence supporting the importance of wellbeing and even more urgency to integrate this evidence into care. Ariadne Labs is working on developing a starting point, one that offers a vision of a new kind of care and some simple stepping stones for moving the culture and practice in long term care facilities towards that goal. Pilot testing of these tools is planned for later in 2022. Visit our website or reach out to learn more.
Rachel Broudy, MD, is the Medical Director of Pioneer Valley Hospice and Palliative Care and lead faculty on Ariadne Labs’ work to reimagine the care of older adults in nursing homes. Dr. Broudy is passionate about building a future where health care for frail elders is based on well-being, where clinical interventions integrate older people more fully into our communities, and where systems of care prioritize and encourage agency, social connection, and sense of purpose.



