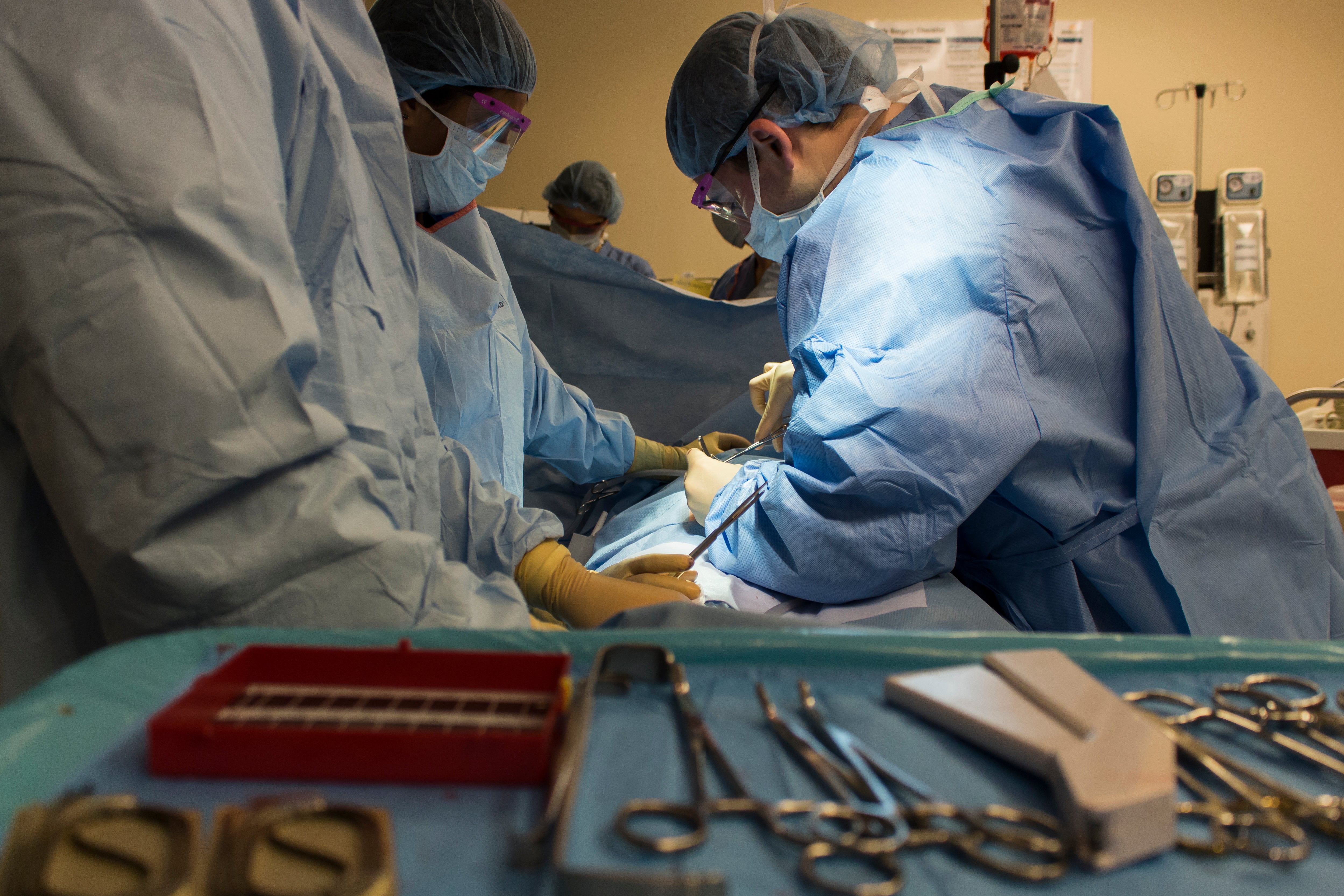
Boston, MA — Employee performance review season is often met with feelings of dread for what can be viewed as an ineffective or unnecessary process. But a new study from Ariadne Labs suggests that for surgeons, feedback from their coworkers may hold greater value than they realize and provide an indicator for the quality of care they provide.
Published in the Annals of Surgery, the study finds that surgeons who receive poor ratings in communication and teamwork skills from their coworkers during 360-degree performance reviews are more likely to face malpractice claims from patients. Specifically, the study looked at performance ratings of service, respect, excellence, personal responsibility to patients, openness, education and humility.
“This is the first study to establish a correlation between performance reviews and malpractice claims,” said lead author Dr. Janaka Lagoo, a surgical research fellow at Ariadne Labs. “The findings suggest that everyday negative conduct by surgeons toward their colleagues can have real implications for care, even when surgeons are highly skilled technically.”
Using data from the CRICO/ Risk Management Foundation of the Harvard Medical Institutions, the study compares claims for 264 surgeons at Harvard-affiliated hospitals with the scores from their 360-degree performance reviews. These reviews incorporate feedback from supervisors, team members and other colleagues. This type of review has long been used in other industries and has become more prominent in the medical field in recent years.
Research has demonstrated a high number of malpractice claims indicates a problem for patient safety, as a surgeon’s actions or behavior may be causing their patients harm. What may be less apparent is that numerous claims are a sign of problems for both hospitals and the individual surgeon. When surgeons have a high number of claims, the hospitals where they work are exposed to greater financial risk. Furthermore, studies have shown these surgeons are more likely to report burnout, depression and thoughts of suicide.
Because of the potential for significant and wide-reaching impact, health systems are keenly interested in identifying and fixing the underlying factors that drive malpractice claims. But what are they? Mistakes in how an operation is performed, often linked to a surgeon’s technical skills, can be one factor. However, poor non-technical skills, like teamwork and communication style, are also associated with bad surgical outcomes and, therefore, more medical malpractice claims. According to a 2015 report from the Risk Management Foundation of the Harvard Medical Institutions, the malpractice insurer for all Harvard-affiliated hospitals, approximately one-third of claims involve a breakdown in communication.
A communication breakdown can be the result of what is not communicated. For example, a provider may not record a patient’s allergies in the medical record, resulting in that patient receiving the wrong medication. However, how a surgeon communicates information also matters. A surgeon may have excellent technical skills in the OR, but if they yell at the rest of the surgical team and show them little respect, it creates an unsafe working environment for the team. That, in turn, according to the authors, creates an unsafe environment for the patient.
“Some surgeons might believe a more aggressive communication style is necessary to protect their patients and ensure good results from their operations,” said Lagoo, “but our work adds to the research showing the opposite to be true.”
The 360-degree reviews used in the study were completed between 2012 and 2013. The study included reviews for surgeons from the departments or divisions of cardiac, thoracic, vascular, plastic, orthopedic and general surgery at eight Harvard-affiliated hospitals. Each surgeon identified 20 to 30 colleagues to complete the performance evaluation. The performance domains — service, respect, excellence, personal responsibility to patients, openness, education and humility — are based on the Harvard Surgery Code of Excellence, the standard of conduct expected of all affiliated surgeons.
The survey used a five-point Likert scale and included both positive statements, such as “behaves in a way that encourages team members’ best work” and “admits when wrong,” as well as negative ones, such as “snaps at others when frustrated.” The evaluators’ ratings were then aggregated into an average score per statement and compared with the number of malpractice claims filed for the given surgeon between 2000 and 2015. The number of claims per surgeon ranged from zero to eight.
Surgeons had a greater chance of incurring at least one claim if they scored in the bottom 10 percent on two items: “snaps at others when frustrated” and “is open to suggestions.”
The study adds to the growing literature around what factors affect patient safety and what can be done to make improvements. “This work builds on previous research from our group that showed the value of 360-degree reviews for surgeons,” said Dr. Alex Haynes, director of Ariadne’s safe surgery program and senior author on the paper. “It highlights that improving communication skills and teamwork are important steps for health systems to take in the overall effort to ensure high quality care for patients.”
While it is unclear if and how easily problematic behaviors can be changed, Lagoo and the study team believe there are potential ways for surgeons to improve their non-technical skills using information from their reviews. One possibility is for hospitals to use a modified, shorter version of the reviews and on a more regular basis.
“This would support ongoing self-reflection for surgeons and allow them to receive regular feedback on whether their behavior is improving,” Lagoo said.


