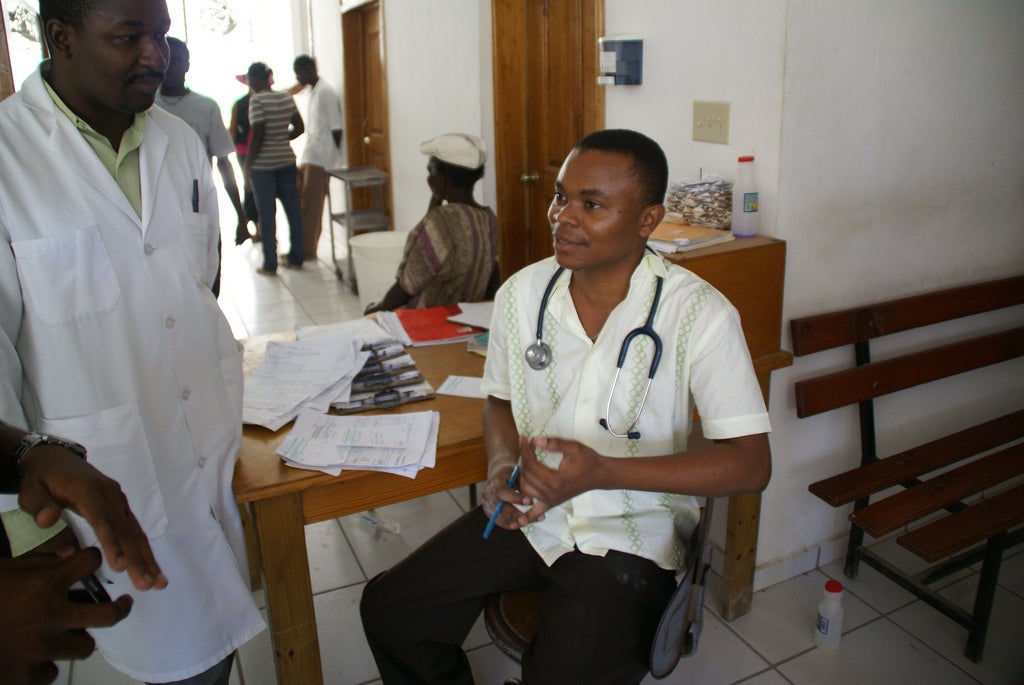
Harvard researchers studying primary health care in Haiti have developed a method of analyzing medical facilities that could help developing nations the world over improve their healthcare services.
The results were recently published in the peer-reviewed journal Bulletin of the World Health Organization. Dr. Margaret Kruk is the study’s senior author and serves as associate professor of global health at Harvard’s T.H. Chan School of Public Health.
The team, led by Dr. Kruk and researcher Anna Gage, included primary health care experts in Haiti as well as Dr. Asaf Bitton, director of the Ariadne Labs primary health care program. They started their study using a set of existing statistics that analyzed healthcare quality at facilities across Haiti. The Western Hemisphere’s poorest country, Haiti has poor health outcomes overall, but in recent years has made progress in lowering mortality rates among children under age five.
For this study, the researchers followed a framework that describes the important components of a strong primary health care system. The framework, which Ariadne Labs helped generate as part of the Primary Health Care Performance Initiative, provided the study team with a set of criteria that allowed them to compare quality measures at Haiti’s primary health care facilities.
The researchers began with Service Provision Assessment (SPA) data collected by the USAID’s Demographic and Health Surveys program, which has measured health care facilities in 11 developing nations. While the data assesses the quality of the facilities, nobody had previously crunched the numbers into usable composite measures, said Anna D. Gage, the study’s first author and researcher with Harvard’s Department of Global Health and Population.
“The motivation of this paper was to first develop a measure of primary care,” Gage said.
The composites they created assess primary health care facilities across areas: access, effective service delivery, organization and management, and provision of core primary health care functions. Among such indicators that made up the composites was whether a facility gathers feedback from patients, something that is done in just 2 percent of Haitian facilities, but is widely seen as a way to improve care. The criteria evaluate facilities on the provision patient care, like whether doctors and nurses take a child’s temperature during an exam or ask a pregnant woman’s age during her initial checkup. The indicators noted whether the facility can perform basic functions such as maintaining client records and appropriate medical waste disposal, which for instance is available at only 37 percent of Haitian healthcare facilities.
What they found was a wide disparity, with rural areas especially having less access to quality medical services – and in some cases lacking services for even basic needs. One key finding: only 5 percent of rural residents but 46 percent of urban residents had access to overall good quality service delivery. Overall, only 2.5 million people of Haiti’s 10.6 million population live within 5 kilometers of a facility with good overall quality of care.
“The big takeaway was the access to quality care isn’t equal,” Kruk said. “Haitians have a lot of clinics and hospitals they can get to, but there are a lot of differences in the quality of care they will find.”
The researchers hope the study can be used to improve Haiti’s substandard healthcare facilities. Previously, system goals often concentrated on opening new facilities to increase access. Now they can hopefully turn to improving the ones that exist, said Bitton, one of the co-authors and a primary care doctor at Brigham and Women’s Hospital.
“The conversation for many years has been, ‘We need more clinics and we need more supplies.” Those things are important, but now it’s time to move beyond numbers of clinics to the quality of care being provided in those clinics,” Bitton said. “It doesn’t help to have a clinic if the healthcare workers aren’t properly trained and motivated to meet patients’ needs.”
With the data crunched through the new criteria, Gage then created a map that shows which areas have the best access to quality care. The work showed rural areas are less likely to offer quality primary care functions, accessible care, effective service delivery, and management and organization.
Along with the researchers from Harvard, the study included three co-authors in Haiti who are now working to get the research in the hands of people who can take measures to improve the substandard clinics and hospitals, Kruk said. “The main audience, we hope, is people running Haiti’s healthcare system,” she said. NGOs and nonprofits working in the country can also use the study to target areas that need the most help.
Now that the researchers have developed the composite criteria, it can be applied to primary health care facilities in other nations, Gage said. Already, identical SPA data exists for countries including Bangladesh, Napal, and Tanzania. It’s possible similar data sets collected elsewhere by other organizations could also be analyzed using the new criteria, Gage said. A new Lancet Global Health Commission on High Quality Health Systems, led by Kruk and Dr. Muhammad Pate, former Minister of State for Health in Nigeria, will examine how this measurement approach can be adapted to a variety of low- and middle-income country settings where primary care has a large but as yet unfulfilled potential for improving health outcomes.
The study may also be the first step toward offering the same kind of composite evaluation for primary health care facilities in developed nations, including the United States. In those cases, researchers could use similar criteria to determine which areas have access to advanced medical care and technology, Kruk said.
“The broader goal of this work is hopefully to clarify the value and performance of primary care globally,” Kruk said. “Clear and robust measures could help countries get beyond using access to care as a measure of success and instead to demand better quality from their primary care systems.”
–By Eric Barton
Cover photo by Alison Wright, 2010. Used with permission.


